Earlier this week, I completed my tenth round of chemotherapy for breast cancer. It’s been a long, exhausting road to get to this point, and to say that I am looking forward to finishing up this part of my treatment would be a gross understatement. I have two more rounds to go, with post-chemo interventions to follow, but, for now, I’m focusing on getting through chemo.
At each round of my chemotherapy treatment, I’ve been accompanied to the hospital, Dana Farber Cancer Institute in Boston, by a friend or my husband; having someone to act as cheerleader, chauffeur, and support system has made a big difference in reminding me I am not alone in my efforts to get better.
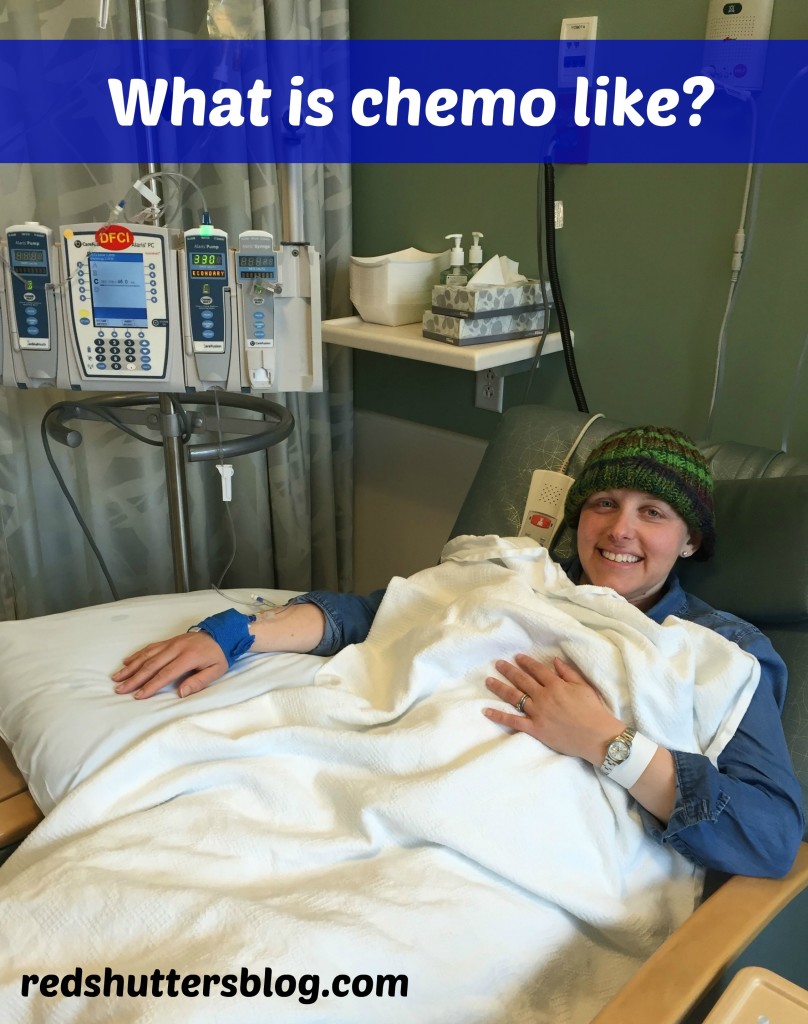
Two of the friends who have escorted me to chemo recently commented how little they knew before they went with me, and how fascinating they found the process. As a science nerd, I understood how they felt. If chemo didn’t make me feel so awful, I might find it fascinating, too. My friends wondered if I would be up for sharing “a day in the life” of my chemo treatment, as it might be a value to others who are chemo novices. What is chemotherapy really like? How does my chemo day go? Today’s post gives you the “behind the scenes” peek at a typical chemo day for me. Please keep in mind that this is my experience; each patient’s journey through chemotherapy is different.
Morning
My chemotherapy is scheduled for a Monday, as I want, as much as possible, to have the days of not feeling good to fall when my kids are in school. I want to preserve the weekends for my family. My oncologist, as a result, recommended Mondays to give me enough time to recover for Saturday and Sunday. I have stuck with that for the past ten rounds.
I usually have chemo in the afternoon, so my mornings are free for the normal stuff of life. I get the kids ready for the day, walk them to school, and chat with my neighbors. Some mornings, if I have energy, I exercise; other days, when I am tired or worn out (which is most of the time), I take it easy. We’re in the midst of a home renovation, so this Monday, I chatted with our contractor before running around the house to cross things off my to do list like the laundry and tidying up the kitchen. Then, I responded to emails, and got showered and dressed in comfortable clothes (leggings and layers are my preferred chemo attire). I also made sure my bag was packed with the items I’d want at the hospital, including my Kindle, a magazine, my wallet, my iPhone, a scarf, as well as a little notebook where I track all of my medical appointments and a folder of documents about my treatment plan. On the weeks when I’m really organized, I also pack snacks, a water bottle, and candy (to get rid of the bad taste in my mouth that can happen during chemo).
Mid-Day
My chemo companion arrives around 11:30 AM; this week, Phyllis, a lovely friend who would have taken me every week if I had let her, accompanied me. We compromised on two rounds of chemo; this is her second visit to DFCI with me. On the drive into Boston, we catch up on life and decide on a restaurant for a pre-chemo lunch.

This week’s chemo companion, the lovely Phyllis of the Napkin Hoarder blog (www.napkinhoarder.com), at lunch at Tiger Mama
A tradition I’ve started is to take my chemo companions out for lunch before we have to report to DFCI for treatment. It’s a small way to say thank you, and it’s a big way to distract myself from what’s to come. Despite my surface cheerfulness, chemo days stress me out. I’m anxious, as most people would be, I think, about the pending treatment, which is why a kind friend is such a balm for my tired out soul. The lunch beforehand is a ritual of sorts, a breaking of bread, to honor what my body is going through. Tiger Mama in the Fenway has been my top choice for this lunch; the food is delicious, and, if the Red Sox are not in town, parking is easy. (If you go, I recommend the Pad Thai.)
Afternoon
Upon arriving at DFCI, the first stop on our chemo tour is laboratory services on the second floor of the Yawkey Center for Cancer Care. Here, I check in for the day, getting a wristband with my name, birthday, and a bar code printed on it; at each point of chemo, the bar code on my wristband is scanned to make sure I am who I say I am. It’s one of the many safeguards DFCI has in place to protect patients. I also get a yellow tracker (which I call a tracker jacker in a homage to the Hunger Games), so DFCI can find me if I’m not where I’m supposed to be. It’s very Big Brother, but it’s another safeguard the hospital uses, and I’m used to it now.

1) My weekly visit to say hi to the Andy Warhol that hangs down the hall from the meditation room; 2) Phyllis and me in the meditation room; 3) This is where I sit to get the IV put in; 4) Phyllis on the move at DFCI.
Laboratory services is my least favorite part of my chemo day – and that’s say a lot since I’m about to fill my body with toxins. At the lab, I get an IV put in so the drugs can be entered directly into my veins. The IV hurts going in; there’s no sugarcoating that. Some patients have a port, which is a tube that’s placed under the skin for chemo infusions, but that method wasn’t recommended for me. Fortunately, you can request the nurse who inserts your IV at DFCI, and I have found two extremely kind and conscientious nurses, Leslie and Cheri, who go out of their way to make me comfortable.
After the IV is inserted on my right wrist and blood taken to make sure my levels were okay for chemo (they are), Phyllis and I head upstairs to the cafeteria to grab iced tea and a chocolate fix. We also visit the meditation room around the corner for some quiet time (no meditation for us, though; we check out Instagram instead). Then, we go up to the ninth floor.
The ninth floor at DFCI is where breast cancer patients are treated. I check in at the front desk, scanning my wristband. Phyllis and I get seats in the sunlit waiting room, scoring People and Entertainment Weekly to read, and wait for my appointment with the nurse practitioner (NP).
I meet with my oncologist or the NP every few weeks. Phyllis waits while I go solo into the appointment, at my request. I have a list of questions written down in my little notebook, and, as a result, I end up taking four pages of notes about a number of issues, including sleep (I’m not getting enough), future appointments (I have radiation starting in a few weeks), and steps I can take to be healthy (sleep, eat well, and exercise). I’ve been doing pretty well throughout chemo, but lately, as the cumulative effects of chemo have been building up in my body, I haven’t felt as well and it’s been rough. Having a chance to talk through my concerns and questions is very beneficial, and I feel better after I leave the appointment. My “homework” for the week, says the NP, is to get more sleep, and I am trying very hard to do so.
After the appointment, I check back in at the front desk for chemo, and Phyllis and I sit on the other side of the waiting room to be called. My primary chemo nurse, Megan, is on vacation, so I am cared for by LeeAnn, another member of the caring team at DFCI. I have been so impressed by the staff at DFCI; everyone – I mean everyone, from the cashier in the cafeteria to the doctors to the front desk staff – is unbelievably kind, and I sense, in this place, a communal commitment to getting the patients better. It makes a difference when you feel like everyone is rooting for you.
To get the chemo underway, I am settled into a chair in the infusion area. Sometimes, I get chilly during chemo, so I am covered up by two warm blankets, as my IV is hooked up to the chemo drugs. Phyllis and I talk (and laugh) non-stop, as LeeAnn gets my treatment started and as she comes back several times to check in on me. It takes about an hour and half to get the pre-drugs (including Pepcid) and the chemo drug into my system. I get one or two drugs, depending upon the week; this week, thankfully, it is only one. I try not to think too hard about the drugs going into my system. I know what they are supposed to do is important – kill off the cancer cells – but they are also intense drugs that are changing so much about me. Generally, I feel okay during chemo, but am very, very tired. The side effects, when they do come, arrive in the next day or two.
And, then we are done. Phyllis and I say good-bye to LeeAnn, and head down to the parking garage. On the ride home, I am a bit queasy, which is normal for me, and worn out, like I had run a long race without any sleep.
Evening
Phyllis drops me off at home around 7 PM; it truly has been a long day. We hug good-bye, and I go inside to say hello to my family. I greet my kids, husband, and mother-in-law who is there to help with the kids. Then, I change into pajamas and get into bed. My husband brings me dinner in bed (he’s a keeper), and exhausted, I fall sleep.
That’s my chemo day.
Overall, it’s tiring. Scary, too. But kindness abounds, and I’m grateful for that.
Two more rounds to go.

Hang in there. The cancer may be zapping your physical strength, but you are still resilient and beautiful.
Thanks for reading and sharing, and for your support, Gail!
Kimberly – take care of yourself- obey Nurses orders and get your sleep and hopefully take some small comfort in knowing there are only two more to go-thinking of you often!
Susie
Will do, Susie!
Kimberly, this is a thoughtful account of the chemo experience. I like that you take the time to have lunch before launching into the treatment. The frequency and number of treatments must feel daunting but you are strong.
I just finished radiation.. I had to go to Weymouth every day. That was the part that wore me out. If you want to talk, please reach out. Thinking of you and sending positive, healing energy.
Maureen
Thanks for your kind words, Maureen, and congratulations to you for finishing radiation!
KImberly my friend, my thoughts are with you. You are one of the strongest people I know. Your strength, beautiful family and friends and lots of TLC and sleep will get you to the other side of this battle.
Thanks for sharing this Kimberly. These stories help inspire those of us who work in research to work even harder. Sending prayers and good thoughts your way.
You are Amazing! Just to compose this blog while feeling the way you do is Phenomenol! Love you!
Oh girl! 2 more rounds and then radiation! You are AMAZING. Amazing for staying so strong, telling every little bit of your story and remaining so positive! You’ve got this! I am always rooting for you! Definitely try to get that much needed rest. Always praying for you!!!!! xo
Kimberly, you are a great sport to put this up online. I am happy 2 more to go and to hear that you have friends and family accompanying you! I wish I could be there to take you and hug you. Continue your battle with strength, humor and love. Thanks for sharing I am always thinking about you and sending love. Happy Mother’s day this weekend, I’m sure Rob and the kids will do something wonderful for their amazing Mom. LOve you Maria
Thank you for sharing your story. You are so brave and I will keep you in my thoughts and prayers.
Sorry you have to go through this. Fingers crossed for a good outcome. Bruce